Team approach to concussion management
"It takes a village to manage a concussion." The brain is one of the most complex organs in the body. It controls our body, thoughts, emotions, memory, and communication. As with many disease and disorders, a multidisciplinary team approach to concussion management is considered best practice. [1, 2]
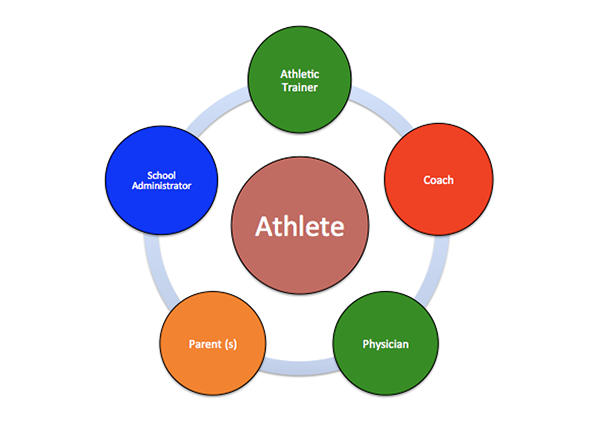
Why is a Multidisciplinary Concussion Management Team approach so important?
A concussion can affect an individual's physical wellbeing, cognitive wellbeing, and emotional wellbeing, therefore professionals from the medical community, educational system, and family members are needed. The collaboration amongst these professional form a team that help determine:
- Symptom management
- Academic progressions or return to learn
- Social and emotional health of the concussed individual
- Return to activity or play
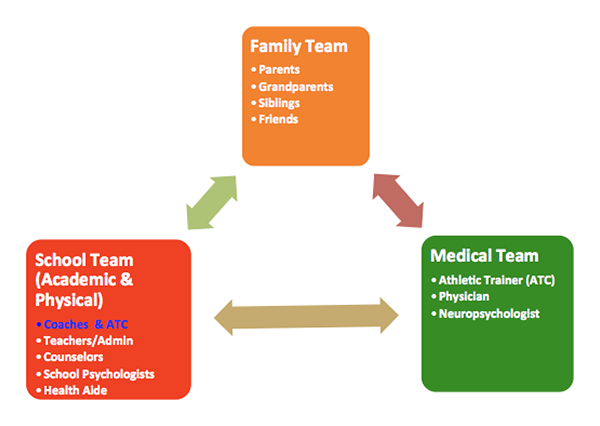
The Multidisciplinary Concussion Management Team should consist of:
- Family team
- Medical team
- School Team
Who is on the Family Team and what is their role on the Multidisciplinary Concussion Management Team?
The Family Team consists of:
- The concussed individual
- The parent or guardian
- Grandparents
- Siblings
- Peers of the concussed individual
The role of the Family Team is to be an advocate for the concussed individual. The Family Team would:
- Notify the school that their child has been diagnosed with a concussion
- Report any observable symptoms
- Report any change in behavior such as irritability, depression, social withdrawal, and/or more emotional then normal.
Who is on the Medical Team and what is their role on the Multidisciplinary Concussion Management Team?
The Medical Team usually consists of:
- Doctor of Medicine or MD
- Doctor of Osteopathic Medicine or DO
- Clinical Neuropsychologist
- Vestibular Therapist
- Physical Therapist
The role of the medical team is to care for the medical and physical needs of the concussed individual. The Medical Team would:
- Provide management strategies for reducing symptoms
- Monitor physical symptoms involving the eyes, cervical spine, and balance
- Prescribe medication when needed
- Review diagnostic tools such as neurocognitive testing and balance
- Prescribe physical and vestibular ocular therapy
- Determine when it is safe to return to play
- Provide written medical clearance
Who is on the School Team and what is their role on the Multidisciplinary Concussion Management Team?
The School Team is further divided into an Academic Team and a Physical team. The School–Academic Team members usually include:
- Student Service Coordinator
- Counselor
- Teacher
- Speech Language Pathologist
- School Psychologist
- Administrators
The role of the School-Academic Team is to provide classroom adjustments and feedback to Medical and Family Team members. The School-Academic Team would:
- Provide classroom adjustments that would help the concussed student control or not exacerbate symptoms.
- Provide classroom and academic adjustments that would help adapt the concussed student be successful in the classroom during recovery.
- May develop an action plan for the concussed student for academic adjustments
- Monitor Progress and share information on teacher observation, symptoms noted during class, and academic performance.
The School-Physical Team members usually include:
- Athletic Trainer (if available)
- School nurse or Health Aid
- Physical Education Teacher
- Coach (usually in high school setting)
- Athletic Director (usually in high school setting)
The role of the School-Physical Team is to :
- Continue to keep concussed student out of physical activity such as physical education classes or sport practice.
- Observe and share information on physical symptoms, mental status and energy/fatigue during the day.
- The athletic trainer may provide computer-based neurocognitive assessments such as ImPact when available
- Administer and Monitor Gradual Return to Play Protocol
The Multidisciplinary Concussion Management Team is the safest and best practice to monitor and manage a concussed individual. The team communicates and collaborates with each other to determine when it is safe to return to play.
The members and involvement of professional will vary according to each concussion case and the resources available. The main point is that the information between the medical, family, and school are communicated and collaborated to determine what is best for the concussed individual.
[1] Halstead, M.E., et al., Returning to learning following a concussion. Pediatrics, 2013. 132(5): p. 948-57.|
[2] Baker, J.G., et al., Principles for return to learn after concussion. Int J Clin Pract, 2014. 68(11): p. 1286-8.


